Advanced Brain Tumor Resection: Modern Surgical Techniques for Safer Tumor Removal

- What Is Advanced Brain Tumor Resection?
- When Is Brain Tumor Resection Recommended?
- Goals of Advanced Brain Tumor Surgery
- Techniques Used in Advanced Brain Tumor Resection
- Surgical Simulation for Brain Surgery: ATLAS Simulation Platform
- Benefits of Advanced Surgical Techniques for Brain Tumor Removal
- Risks and Possible Complications of Brain Tumor Resection
- Recovery After Advanced Brain Tumor Resection
- Why Surgical Expertise Matters in Complex Brain Tumor Surgery
- Frequently Asked Questions
- Key Takeaways
- Getting There
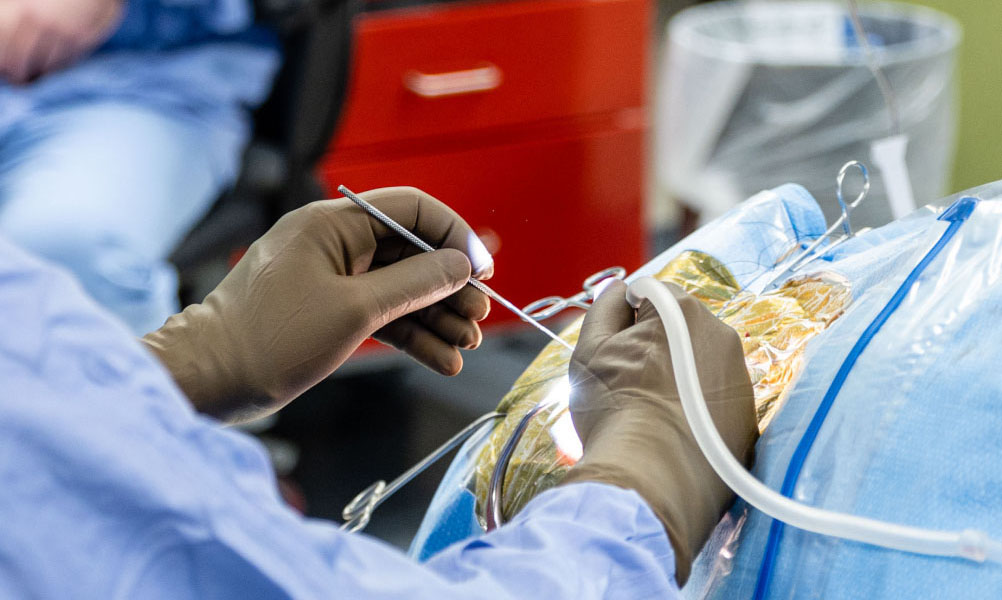
A brain tumor diagnosis can be overwhelming, but advances in neurosurgical technology have significantly improved treatment outcomes for many patients. Advanced brain tumor resection (surgical removal) represents the modern evolution of brain tumor surgery, combining sophisticated imaging, surgical planning, and minimally invasive techniques to remove tumors as safely and effectively as possible.
For many patients, advanced brain tumor resection offers the best opportunity to remove or reduce tumor burden, relieve symptoms, and improve long-term outcomes. Understanding how these advanced techniques work can help patients feel more confident about the surgical process and what to expect during treatment.
What Is Advanced Brain Tumor Resection?
Advanced brain tumor resection refers to the surgical removal of a brain tumor using modern technologies and specialized techniques designed to maximize tumor removal while protecting vital brain structures.
In the past, brain tumor surgery relied primarily on a surgeon’s anatomical knowledge, limited imaging tools, and large incisions. Today, advanced brain tumor resection integrates cutting-edge technologies such as surgical simulation, neuronavigation, intraoperative imaging, and brain mapping. These innovations enable surgeons to operate with exceptional precision while preserving healthy brain tissue and critical neurological functions.
Brain tumor resection is often the primary treatment for many types of tumors, including benign (noncancerous) and malignant (cancerous) growths.
The brain is a highly complex organ responsible for essential functions such as movement, speech, memory, and vision. Because tumors can develop near the areas that control these critical functions, surgery requires a highly precise and carefully planned approach.
Advanced neurosurgical techniques enable surgeons to:
- Identify and remove tumor tissue more accurately
- Navigate complex brain anatomy safely
- Preserve neurological function
- Reduce the risk of surgical complications
By combining surgical expertise with modern tools, advanced brain tumor resection enables surgeons to treat tumors that were once considered extremely difficult or even impossible to remove.
When Is Brain Tumor Resection Recommended?
Not every brain tumor requires surgery. Some tumors grow slowly and can be monitored through regular imaging. However, resection is commonly recommended in several situations.
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.
Tumors That Cause Neurological Symptoms
When a tumor presses on surrounding brain tissue, it can cause symptoms such as the following:
- Persistent headaches
- Seizures
- Vision changes
- Difficulty speaking
- Weakness or numbness
- Balance problems
Removing the tumor can relieve pressure on the brain and improve these symptoms.
Uncertain Diagnosis
Surgery might be necessary to obtain a tissue sample that enables doctors to determine the exact type and grade of the tumor.
Rapid Tumor Growth
Aggressive tumors often require prompt surgical removal to prevent further spread or damage to surrounding brain tissue.
Tumor Accessible for Removal
If imaging studies show that a tumor can be removed safely, advanced brain tumor resection might provide the best chance for long-term control.
The decision to proceed with surgery depends on factors such as the tumor’s location, size, and type, and the patient’s overall health.
Goals of Advanced Brain Tumor Surgery
The primary goal of advanced brain tumor resection is to remove as much of the tumor as safely possible while protecting the patient’s neurological function. Surgeons typically focus on several key objectives.
- Maximum safe tumor removal: Removing the entire tumor can provide the best chance for cure for patients with a benign tumor and improve survival in those with a malignant tumor.
- Preservation of brain function: The brain controls many vital functions, so protecting the areas responsible for speech, movement, and memory is critical.
- Accurate diagnosis: Tumor tissue obtained during surgery allows pathologists to identify the type of tumor and determine the most effective follow-up treatment.
- Improved effectiveness of additional treatments: Removing a large portion of a tumor can make radiation therapy or chemotherapy more effective.
By planning the surgery carefully and using advanced surgical tools, surgeons can balance tumor removal with preservation of the patient’s quality of life.
Techniques Used in Advanced Brain Tumor Resection
Modern neurosurgery incorporates several innovative techniques that enhance precision and safety during advanced brain tumor resection.
These tools enable surgeons to see the tumor more clearly, navigate nearby complex brain structures, and monitor brain function throughout the procedure.
Surgical Simulation for Brain Surgery: ATLAS Simulation Platform
Dr. Aaron Cohen-Gadol uses one of the most advanced surgical simulation platforms available today—the proprietary ATLAS Simulation technology—to create a highly realistic, patient-specific “virtual twin” of the patient’s brain.
This powerful system enables him to rehearse the entire operation before entering the operating room. Using detailed magnetic resonance imaging (MRI) and other imaging data, the ATLAS platform generates a 3-dimensional model of the patient’s tumor and unique brain anatomy.
In this virtual environment, Dr. Cohen-Gadol can carefully evaluate the safest and most effective pathway for removing the tumor, particularly when it is located in a delicate or difficult-to-reach area.
The process is similar to that followed by fighter pilots who are trained using high-resolution simulators before performing complex missions. Pilots practice maneuvers in a risk-free environment so that they can respond effectively in real-world situations.
In the same way, surgical simulation allows Dr. Cohen-Gadol to:
- Study the patient’s individual anatomy in detail
- Test multiple surgical approaches
- Identify potential challenges
- Refine the surgical strategy
By practicing the operation beforehand, he can optimize tumor removal while minimizing risk to healthy brain tissue and essential functions such as speech, movement, and vision.
This type of detailed preparation represents one of the most innovative aspects of advanced brain tumor resection today.
Awake Brain Surgery (Awake Craniotomy)
Awake craniotomy is a specialized technique used when a tumor is located near a critical brain area responsible for speech, movement, or memory.
During this procedure, the patient is awake for part of the surgery so that the surgical team can monitor neurological function in real time. The patient could be asked to perform tasks such as speaking, counting, or moving certain limbs while the surgeon carefully removes tumor tissue.
This approach helps surgeons avoid damaging essential brain regions.
Intraoperative Brain Mapping
Brain mapping is another powerful tool used during advanced brain tumor resection. Using small electrical stimulations, surgeons identify areas of the brain responsible for important functions such as speech, motor control, and sensory processing.
By mapping these areas during surgery, surgeons can remove tumor tissue while preserving critical neurological pathways.
Image-Guided Neuronavigation
Neuronavigation systems function like GPS for the brain. During advanced brain tumor resection, these systems combine preoperative imaging with real-time surgical data to guide the surgeon to the tumor with extreme accuracy.
This technology helps surgeons track their instruments within the brain and ensures precise tumor removal.
Intraoperative MRI and Ultrasound
Imaging tools used during surgery can help surgeons confirm how much tumor has been removed.
Intraoperative MRI or ultrasound enables doctors to view updated images of the brain during a procedure, which can reveal residual tumor tissue that might not have been visible initially.
This real-time imaging improves the effectiveness of advanced brain tumor resection.
Benefits of Advanced Surgical Techniques for Brain Tumor Removal
Modern techniques used in advanced brain tumor resection provide several important advantages for patients.
- Greater surgical precision: Advanced imaging and navigation technologies enable surgeons to operate with exceptional accuracy.
- Increased tumor removal: Better visualization and real-time imaging help surgeons remove more tumor tissue when it is safe to do so.
- Preservation of brain function: Techniques such as awake surgery and brain mapping protect critical neurological functions.
- Reduced surgical risk: Careful planning and the use of advanced tools can lower the risk of complications.
- Improved treatment outcomes: More complete tumor removal can improve survival rates and enhance the effectiveness of additional treatment(s).
These benefits have made advanced brain tumor resection a cornerstone of modern brain tumor treatment.
Risks and Possible Complications of Brain Tumor Resection
Although advanced brain tumor resection is performed using highly precise techniques, all brain surgeries come with potential risks.
Possible complications include the following:
- Infection
- Bleeding
- Seizures
- Stroke
- Neurological deficits
- Swelling of brain tissue
The specific risks depend on factors such as the location and type of tumor and the patient’s overall health. Working with an experienced neurosurgeon significantly reduces the likelihood of serious complications.
Recovery After Advanced Brain Tumor Resection
Recovery after advanced brain tumor resection varies depending on the complexity of the procedure and the patient’s condition.
Hospital Stay
Most patients remain in the hospital for several days after surgery so that doctors can monitor their neurological function and healing.
Early Recovery
Common temporary symptoms during early recovery include the following:
- Fatigue
- Headaches
- Mild swelling
- Difficulty concentrating
These symptoms typically improve over time.
Rehabilitation
Some patients benefit from rehabilitation programs such as the following:
- Physical therapy
- Occupational therapy
- Speech therapy
These services can help patients regain strength and neurological function.
Follow-up Care
After brain tumor resection, follow-up appointments and imaging scans are important for monitoring recovery and detecting any tumor recurrence.
Why Surgical Expertise Matters in Complex Brain Tumor Surgery
The success of advanced brain tumor resection depends heavily on the skill and experience of the neurosurgeon performing the procedure.
Dr. Cohen-Gadol is an internationally recognized neurosurgeon who specializes in treating complex brain tumors with advanced microsurgical techniques. His practice focuses on maximizing tumor removal while preserving neurological function and quality of life.
Dr. Cohen-Gadol combines deep anatomical expertise with advanced technologies such as surgical simulation, neuronavigation, and intraoperative brain mapping. His use of the ATLAS Simulation platform enables him to carefully rehearse complex procedures and plan the safest surgical approach for each patient.
Patients benefit from his:
- Extensive experience treating complex brain tumors
- Use of advanced surgical planning and simulation
- Personalized treatment strategies
- Commitment to patient education and compassionate care
This combination of expertise and innovation helps ensure the highest standard of care for anyone undergoing advanced brain tumor resection.
Frequently Asked Questions
Can a stage 4 brain tumor be removed?
Some stage 4 brain tumors can be removed completely or partially, depending on the tumor’s location and characteristics. In many cases, advanced brain tumor resection focuses on removing as much tumor tissue as safely possible to reduce symptoms and improve the effectiveness of treatments such as radiation therapy or chemotherapy.
What are the odds of surviving brain tumor removal?
Survival rates vary widely depending on the type of tumor, its location, and how much of it can be removed. Patients with a benign tumor often have an excellent outcome after surgery, whereas those with a malignant tumor might require additional treatment. Advanced brain tumor resection techniques and technologies have improved survival rates for many patients by enabling more precise and complete tumor removal.
What is the hardest brain tumor to remove?
Tumors located near critical brain structures, such as the brainstem, deep brain regions, or areas responsible for speech or movement, can be particularly challenging to remove. These tumors often require highly specialized techniques and careful planning to treat effectively.
How long does brain tumor resection take?
The time it takes to perform an advanced brain tumor resection varies depending on the size and location of the tumor. Many procedures take between 3 and 8 hours, although more complex surgeries can take longer.
Key Takeaways
Advanced brain tumor resection represents a major advancement in modern neurosurgery. By combining innovative technologies, surgical simulation, and refined microsurgical techniques, surgeons can treat complex brain tumors with greater precision and safety than ever before. For many patients, advanced brain tumor resection offers the best opportunity to remove their tumor effectively while protecting the brain functions that matter most.
Getting There
The clinic is located at Cedars Towers East which is at 8631 W 3rd Street, Suite 815E, Los Angeles, CA 90048, near Beverly Grove. It’s easily accessible from San Vicente Boulevard or La Cienega Boulevard. Paid parking is available in the adjacent structure and limited street parking can be found nearby. For navigation, entering “8631 W 3rd St” into the GPS will direct you to the main entrance.
The entrance to the Cedars Towers East parking garage is on Sherbourne Drive, located just north of 3rd Street. It is a self-parking garage with the address 217 S Sherbourne Dr, Los Angeles, CA. The entrance is on the right if you are traveling south on Sherbourne, or on the left if you are traveling north on Sherbourne. You then need to take the parking elevators to the plaza level and then cross the short bridge to use the East elevators to reach the 8th floor (suite 815.) Allow extra time for traffic and parking, especially during weekday mornings.











