Overview of Arteriovenous Malformation Types

An arteriovenous malformation (AVM) is an abnormal tangle of blood vessels linking arteries and veins directly, without the normal capillary network in between. This causes several problems. In the absence of the fine branching blood vessels of capillaries, blood rushes from the high-pressure artery to the low-pressure vein and bypasses surrounding tissues. Strong turbulent blood flow from the artery can cause the receiving vein to become engorged and rupture.
Brain AVM rupture results in a type of brain bleed called intracerebral hemorrhage and/or subarachnoid hemorrhage. This is a life-threatening condition that can cause a stroke or permanent brain damage. Once an AVM is diagnosed, there are several treatment options available. Prompt management and a comprehensive evaluation of the AVM by an experienced and skilled neurosurgical team is important for the best possible outcomes. Read on to learn more about AVMs.

Figure 1: A large AVM with engorged veins.
Types of AVM
AVMs can be located within the brain (parenchymal AVM) or around the brain in its tough membranous covering called the dura (dural AVM or arteriovenous fistula). Cavernous malformations, venous malformations, and capillary telangiectasias are commonly thought of as subcategories of AVM but are each their own distinct entity and fall under the more general category of vascular malformations.
Importantly, AVMs are commonly graded using the Spetzler-Martin grading scale. This considers an AVM’s size, location, and blood vessels involved to estimate the risk of surgery and is an important tool for determining which treatment option is best. Low-grade AVMs that are smaller and located closer to the surface of the brain are typically easier and safer to surgically remove. More information about the different types of AVMs can be found here.
Symptoms of AVM
Patients of any age can experience AVM symptoms; however, they commonly do so between the ages of 20 and 40. The severity of these symptoms can vary depending on the location and size of the AVM as well as the presence of rupture and hemorrhage.
Nearly half of patients with a brain AVM will experience no symptoms until rupture. Symptoms of hemorrhage can include a sudden and severe headache, nausea and vomiting, loss of consciousness, and other motor and sensory impairments.
Seizure and headaches are general symptoms that also may arise. Other symptoms will vary depending on the location of the AVM. For example, AVMs that neighbor certain nerves may cause pain, whereas AVMs that occur in the back of the head near brain tissues involved in vision processing may lead to vision problems.
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.
Diagnosing AVM
After considering all symptoms, your physician will conduct a physical examination and imaging tests to rule out any other causes. A bruit, or the rushing sound made by blood moving quickly through its vessels, may be discovered on physical exam if the AVM is located near the skin. It can sound like water running through a pipe, and if severe enough, this can be audible to the patient and disturb sleep.
The sudden headache and associated neurological symptoms is usually evaluated emergently in the emergency room via a CT scan.
Diagnosis is confirmed via imaging due to AVM’s characteristic appearance. The following tests are used to detect and evaluate an AVM:
- Computerized Tomography (CT) Scan: This test uses x-rays to visualize the brain and its bony structures and determine if any acute bleeding has occurred. It can also demonstrate any calcifications if present within the AVM. This test is quicker than an MRI but is less sensitive at finding an AVM especially if it has not bled.
- Magnetic Resonance Imaging (MRI): This test uses magnetic fields and radio waves to produce more detailed images of the soft tissues of the brain. The lesion and its surroundings can be assessed more closely to differentiate an AVM from other entities such as a brain tumor.
- Cerebral (Catheter) Angiography: This test involves injecting a water-soluble dye (contrast) into an artery then taking x-rays to highlight the blood vessel structure and pattern of blood flow. This test can identify the exact location of AVM and the blood vessels involved.
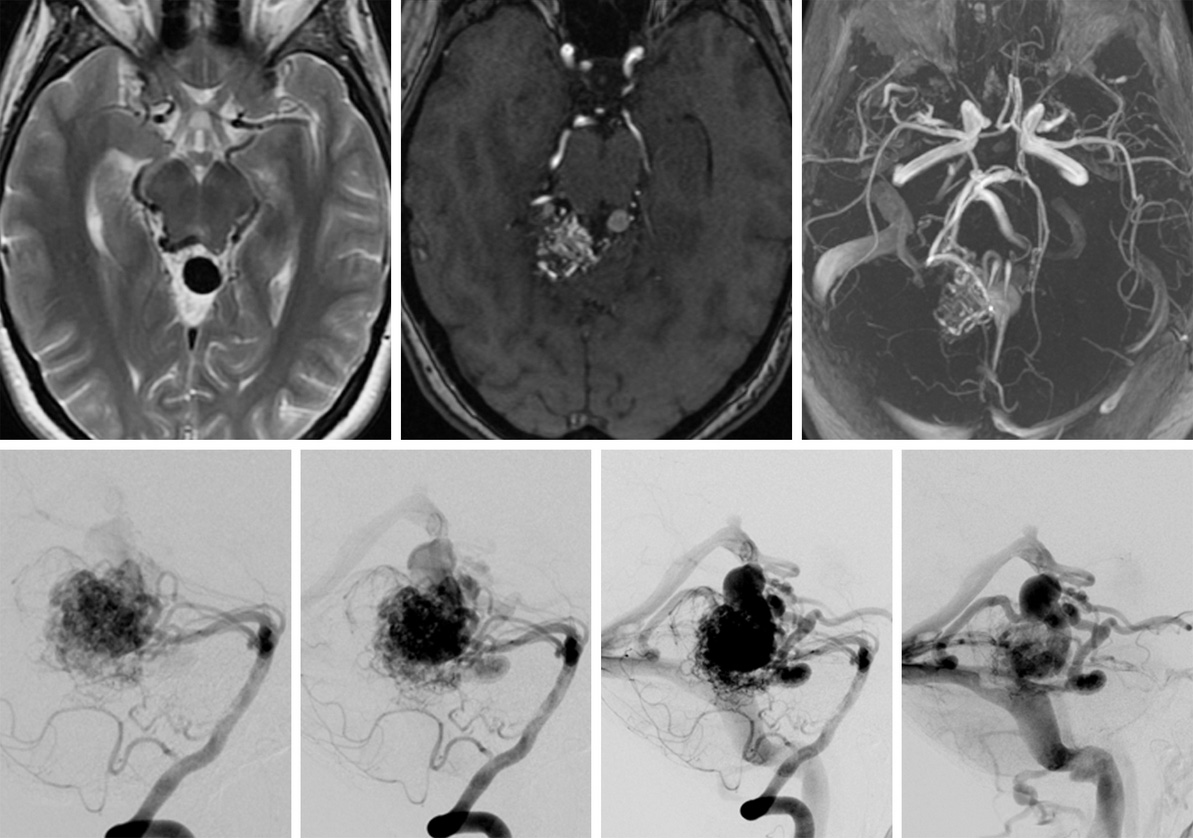
Figure 2: Magnetic resonance (top left) and magnetic resonance angiographic (top middle and top right) images of a brain AVM. Angiographic images of blood flow as it passes from arteries to veins (bottom left to right).
Causes of AVM
Brain AVMs are assumed to form due to mutations that occur during fetal development, but the exact cause is unknown as some patients develop an AVM during their life. Certain genetic factors can contribute to AVM formation and are associated with inherited conditions such as hereditary hemorrhagic telangiectasia (HHT), also known as Osler-Weber-Rendu syndrome.
Conclusion
An AVM is a rare medical condition that affects the arteries and veins. The decision to treat this condition depends on several factors with the primary goal of preventing AVM rupture and minimizing the risk of neurological complications. Your neurosurgeon will discuss the specifics of your AVM and other considerations to determine the best course of therapy.
Key Takeaways
● An arteriovenous malformation (AVM) is an abnormal tangle of blood vessels linking arteries and veins directly, without the normal capillary network in between.
● Often times AVMs are discovered only when they rupture.
● Diagnosis is confirmed through imaging tests.
● The causes of AVM are unknown, although some genetic factors may increase the risk.











