Trigeminal Neuralgia: What the Patient Needs to Know

What Is Trigeminal Neuralgia?
Trigeminal neuralgia is a chronic condition causing shock-like extreme pain in the face, usually one side of the jaw or cheek set off by triggers related to facial pressure and motion. Although the pain is short and intermittent (a typical attack can last anywhere from a few seconds to a couple of minutes), it is extreme and can be incapacitating.
The attacks of pain generally occur together and may repeat in succession, taking place sporadically over the course of days, weeks, or months. Episodes of repeated attacks can be separated by asymptomatic periods for months or even years.
What Causes Trigeminal Neuralgia?
The most common cause of trigeminal neuralgia is compression of the trigeminal nerve (also called the fifth cranial nerve) by an artery or vein at the base of the brain behind the ear. Compression from the blood vessel causes the myelin sheath (a special coating around a nerve that helps it transmit signals faster through the body) to wear down and the nerve to send abnormal pain signals to the brain.
Trigeminal neuralgia is also associated with multiple sclerosis and other disorders that affect the myelin sheath, as well as nerve compression by a tumor.
The pain is generally set off by triggers related to facial pressure or motion, such as:
- Eating
- Drinking
- Shaving
- Talking
- Smiling
- Brushing your teeth
- Applying makeup
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.
Who Is Affected by Trigeminal Neuralgia?
Trigeminal neuralgia can occur at any age, but it is more common among those older than 50 years. In general, women are affected more than men.
What Are the Symptoms?
Trigeminal neuralgia is usually associated with episodic intense sharp, shock-like and electrical pains in the face. The pain is generally felt on one side of the jaw or cheek, although it may occur occasionally around the eye. Less commonly, the pain can also present in other areas innervated (supplied with nerves) by the trigeminal nerve, such as the lips, teeth, gums, or forehead.
The bouts of pain are triggered by some form of vibration or contact (see previous section).
The pain is often described as incapacitating, and it occurs in attacks that last from several seconds up to 2 minutes. The attacks can occur in rapid succession or spaced more sporadically over the course of days, weeks, or even months. The periods of time during which the attacks are prevalent are referred to as episodes. Patients mith have long asymptomatic (pain-free) periods between episodes that last for months or years.
Before the onset of an episode, patients might experience warning signs such as a numb feeling or a chronic aching pain in the areas of the face innervated by the trigeminal nerve.
As time goes on, the attacks usually become more frequent and intense.
How Is It Diagnosed
To diagnose trigeminal neuralgia, a physician will take your history and perform a physical examination. Clinical history is the key component in the diagnosis of trigeminal neuralgia.
Trigeminal neuralgia must be differentiated from atypical facial pain. In atypical facial pain, the pain is more burning, nonepisodic (constant), and not in a specific distribution corresponding to the trigeminal nerve. Atypical facial pain does not respond to the surgical treatments designated for patients with typical trigeminal neuralgia.
If the patient is suffering from trigeminal neuralgia, the physician can order a magnetic resonance imaging (MRI) scan to look for the blood vessel compressing the nerve or to rule out multiple sclerosis or a tumor as the cause of trigeminal neuralgia.
Additional tests can be ordered to rule out other possible causes of face pain.
What Are the Treatment Options?
Medications are the most common initial treatment, although their effectiveness may diminish over time. Medications used include anticonvulsants (for example, Tegretal or Neurontin), muscle relaxants, and tricyclic antidepressants. Tegretal and Neurontin are the first line of medical therapy. Temporary relief of pain after administration of these 2 drugs further solidifies the diagnosis of trigeminal neuralgia.
Anticonvulsants block nerve firing to control pain. However, these medications can have several unpleasant side effects (such as confusion, drowsiness, and nausea) that should be discussed with your physician before you take them. The use of Tegretal requires careful monitoring of your blood count and salt by your family doctor for the first few weeks of use. This monitoring requires a blood test.
Muscle relaxants can be used on their own or in conjunction with anticonvulsants to treat pain. Tricyclic antidepressants are used specifically to treat pain described as constant, burning, or aching.
No patient should live with the severe pain of trigeminal neuralgia. We recommend early consultation with a neurosurgeon if the medications are not effective or if you have unpleasant side effects from them.
Your surgeon may suggest one of many different surgical options, including:
- Microvascular decompression
- Glycerol injection
- Balloon compression
- Radiofrequency thermal lesioning
- Stereotactic radiosurgery
The above procedures fall into 2 main categories:
Physiologic
Microvascular decompression: Usually reserved for patients younger than 70 years, it is more invasive because it requires surgery (craniotomy, removing a small piece of skull and going around the brain to decompress the nerve). This procedure is the most definitive and durable procedure for relieving the pain.
Ablative
The other procedures mentioned earlier, including glycerol injection, balloon compression, radiofrequency thermal lesioning, and stereotactic radiosurgery. These procedures do not require surgery and cause trigeminal nerve injury (numbness) so the nerve does not cause more pain. The primary problem with these procedures is that the compressive artery is not addressed. And while these procedures pose less of a risk to the patient than surgery, the risk of pain recurrence is also higher.
Microvascular Decompression
Microvascular decompression avoids directly damaging the trigeminal nerve and is the procedure with the lowest probability of pain returning in the future. The patient is put completely general anesthesia, and the surgeon enters the head through an incision made behind the ear. A small piece of skull is removed. Using a surgical microscope, the surgeon locates the blood vessels compressing the nerve and gently separates them from the nerve.
A piece of Teflon padding is placed between the nerve and offending blood vessels to prevent further compression of the nerve (see surgical video). This technique stops further pain in most patients (90%), and because the nerve is not damaged, there is generally no permanent facial numbness. The risk of pain recurrence within 5 years is less than 10%.
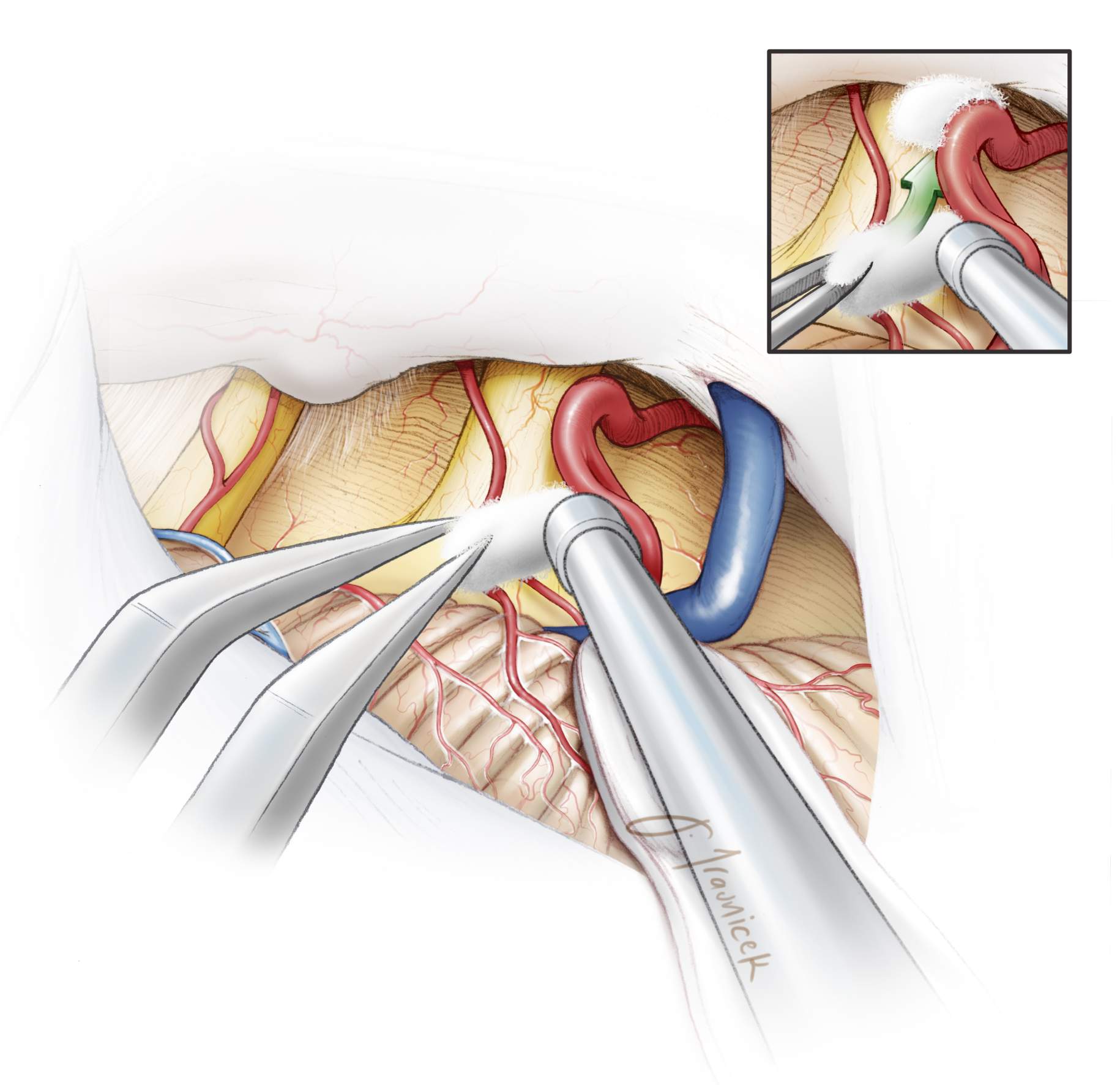
Decompression of the Trigeminal Nerve Using Teflon Padding
As with all surgeries, there are possible complications, and patients very rarely (less than 5% of the time) experience facial weakness, numbness, double vision, or decreased hearing.
In instances where the surgeon is unable to find a blood vessel pressing on the nerve during a microvascular decompression procedure (about 10%–20% of the time), the surgeon might cut part of the trigeminal nerve; if this is done, the patient will be most likely be relieved of his or her facial pain but will experience permanent numbness in the area of the face having pain.
After the surgery, the patient is monitored in the intensive care unit overnight and is then transferred to a private, less monitored floor the next day. Nausea and slight dizziness might be temporarily present (1–2 days). After approximately 2 to 3 days of hospitalization, the patient returns to his or her daily activities and may resume driving in 1 week. Heavy physical activity should be avoided for 6 weeks, and patients with a less physically demanding job can return to work within 2 weeks.
In this video, Dr. Cohen describes the techniques for surgery to treat trigeminal neuralgia using microvascular decompression.
For more information about the technical aspects of the surgery and extensive experience of Dr. Cohen, please refer to the chapter on Microvascular Decompression for Trigeminal Neuralgia in the Neurosurgical Atlas.
Glycerol Injection
Glycerol injection is an outpatient procedure using glycerol to damage the nerve and block pain signals. The patient is sedated, and a needle is inserted through the face toward the base of the skull. The needle is carefully guided to the point where the trigeminal nerve divides into its 3 branches, and a small amount of glycerol is injected around the nerve. The damage caused to the nerve by the glycerol blocks pain signals; some patients experience numbness and tingling as a result of the procedure. The risk of pain recurrence in 5 years is approximately 30%.
Balloon Compression
Balloon compression likewise damages the trigeminal nerve in an attempt to block the pain signals traveling to the brain. A needle is inserted through a small incision in the cheek toward the trigeminal nerve at the base of the skull. A small balloon is threaded through the needle and inflated to compress the nerve against the skull bone.
After approximately 1 to 2 minutes, the balloon is deflated and removed. The pressure from the balloon damages the nerve, inhibiting the abnormal signaling that causes the pain. Balloon compression is generally an outpatient procedure. Patients may experience some degree of facial numbness. The risk of pain recurrence in 5 years is approximately 30%.

The Operating Room Setup for Balloon Compression Rhizotomy
Radiofrequency Thermal Lesioning
Radiofrequency thermal lesioning involves more selective damaging of the trigeminal nerve. The patient is sedated, and a hollow needle is inserted through a small incision in the cheek to where the nerve exits the base of the skull. The patient is awakened, and using an electrode threaded through the needle, the surgeon gently stimulates the nerve at different positions, causing a mild tingling sensation in the different areas of the face innervated by the trigeminal nerve.
The patient is asked to identify when the tingling occurs in the area typical of pain attacks. The patient is then resedated, and the electrode is heated to damage the nerve fibers associated with the pain. Additional lesioning of the nerve might be necessary to completely eliminate the pain. Most people who undergo radiofrequency thermal lesioning experience some degree of facial numbness afterward. The risk of pain recurrence in 5 years is approximately 30%.

Radiofrequency Thermal Lesioning
Stereotactic Radiosurgery
Stereotactic radiosurgery is a noninvasive procedure using high-energy radiation to damage the nerve as it exits the brainstem. The patient has a head frame placed on his or her head on the day of procedure. After the administration of radiation, which takes about 2 hours, the head frame will be removed at the end of the day, and the patient is discharged.
There is minimal pain involved with the procedure itself and extensive anesthesia is typically not used. Patients usually leave the hospital the same day.
Lesioning is slow, and it can take several weeks to months for the facial pain to begin to subside. The rate of recurrence within 5 years is about 50%.
What Is the Recovery Outlook?
Trigeminal neuralgia is not fatal, but the pain can be incapacitating, and without medical intervention, the pain will continue episodically throughout life. This disorder can be managed or cured through the use of medication or surgery. There is a risk that the pain will return later in life.
Resources
National Institute of Neurological Disorders and Stroke
National Institute of Neurological Disorders and Stroke (additional information)
Medline Plus
Mayo Clinic











