Surgery for Arteriovenous Malformation

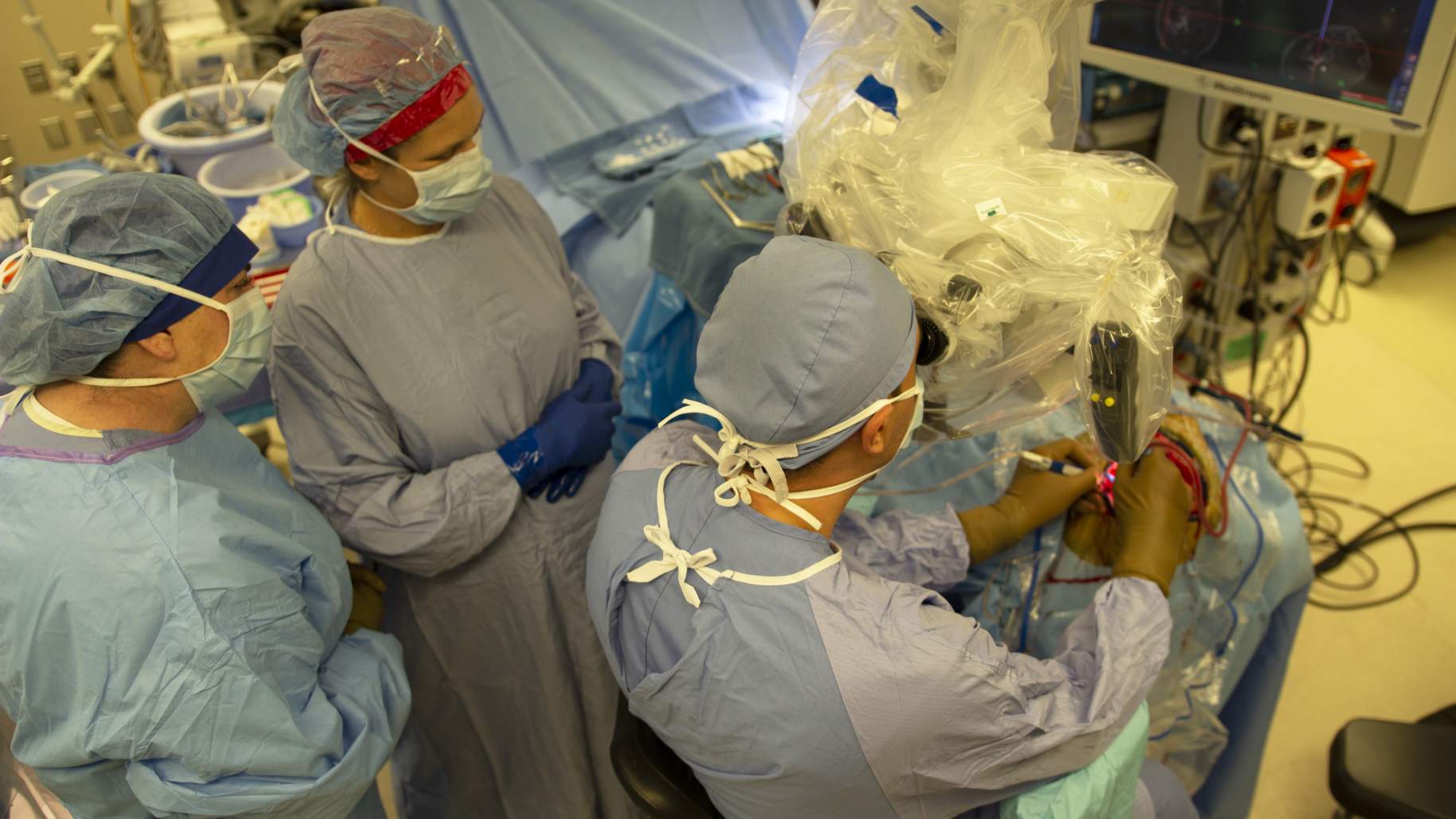
Figure 1: The neurosurgical team working on removal of an AVM using a microscope.
An arteriovenous malformation (AVM) is a tangle of abnormally developed blood vessels that are unable to transfer oxygen and nutrients to the surrounding brain tissues due to the direct connections between arteries and veins without intervening capillaries.
Initial surgical attempts to treat AVMs were discouraging due to their complexity and deep location. However, our understanding of these lesions has remarkably evolved, allowing for significant advances in treatment options including safe surgical removals.
The management of patients with AVMs is complex. How and when to treat an AVM is based on a comprehensive understanding of the natural course of the disease without treatment and the potential risks of intervention. The main goal of treatment is prevention of future AVM hemorrhage and neurological deterioration. The treatment options for AVMs are unique to each patient and can involve a combination of approaches. In the following sections, we will discuss the surgical approach for the treatment of AVMs or Surgery for AVM (Figure 1).
Timing for Surgery for AVM
In general, surgery is performed as an elective procedure unless the AVM has ruptured and caused a blood clot in the brain that is pushing pressure on the surrounding normal brain. The decision regarding if and when to operate are made by taking into consideration both the patient’s symptoms, imaging findings, as well as the neurosurgeon’s recommendations.
Importantly, if a patient presents with a bleed within the brain due to a ruptured AVM, the timing of Surgery for AVM depends on the patient's neurological condition. If, after rupture, the patient is neurologically stable, surgery can be performed in a delayed fashion. The risk of rebleeding after the initial rupture is relatively low, though highest in the first year with an estimated occurrence in 6 – 15% of cases.
On the other hand, if an AVM rupture causes a life-threatening condition due to a large blood clot in the brain, surgery is performed emergently with the primary goal of blood clot evacuation. In this case, the AVM may be removed in the same surgery or left alone for another surgical session. However, if the location and configuration of the AVM are favorable for immediate resection, complete removal can be pursued at the same setting during the emergent surgery for clot removal.
Essential factors in the treatment decision making process include the patient’s age, presence of other medical conditions, and characteristics of the AVM and blood clot such as their size, accessibility, and proximity to critical brain structures. A neurosurgical team that can perform a comprehensive evaluation is recommended to optimize treatment outcomes and recovery.
Surgical Technique
The surgical approach aims to remove the AVM while preserving healthy brain tissue. Although the procedure is performed with the smallest incision possible in the brain, this may still mean that a relatively large incision is made on the scalp and skull bone to provide an adequate exposure of the brain for successful identification of the blood vessels involved with the AVM.
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.

Figure 2: The outline of incision (red hashed line) and craniotomy (skull bony cuts, black line) for a left frontal AVM.
Before the procedure, the surgeon reviews the imaging tests in detail to plan the best surgical approach. Typically, patients undergo an imaging test called intraoperative angiography which allows for direct visualization of the location and blood vessels involved in the AVM. During the surgical procedure, the patient is under general anesthesia and positioned on the operating room according to the location of the AVM.
Once the AVM is reached, the surgeon seals the arteries and veins that are abnormally connected to the AVM, removes the AVM, and redirects blood flow to normal blood vessels. In some cases, patients undergo endovascular embolization before surgery to decrease blood flow to the AVM as much as possible. This two-step approach favors a complete resection.

Fig 3: Exposure of an AVM during surgery under the microscope. Note the tangle of blood vessels and large abnormal draining veins.
The surgery is performed in well-established steps, mainly guided by a microscope. Once the feeding arteries to the AVM are located, they are coagulated and sectioned. The surgeon ensures that all the feeding vessels are identified and uses different techniques to distinguish normal blood vessels from abnormal ones. After all the feeding arteries have been sacrificed, the AVM is resected in a circumferential fashion while avoiding damage to all the healthy brain tissue around it.
Dissection continues with several techniques depending on the location of the lesion. After complete dissection of the AVM, veins are visualized to ensure they do not receive abnormal arterial blood anymore. Next, the surgical field is thoroughly inspected for any residual AVM tissue. If none is detected, the surgery is completed with closure, the bone of the skull is fixed back and the scalp is sutured close. Finally, another angiogram is completed at the end of the surgery or sometime before the patient is discharged from the hospital to confirm complete AVM resection.

Figure 4: The angiography suite.
Surgery Outcomes for AVM
The most commonly used grading scheme to predict the risk and outcomes of surgery is the Spetzler-Martin grading scale. The Spetzler-Martin scale scores an AVM by its size, proximity to critical (“eloquent”) brain tissues, and whether venous drainage is more superficial or deep. A lower score or grade is associated with better outcomes. Other critical information to consider include the age of the patient, whether bleeding is present, and the compactness of the AVM.
In patients with low-grade AVMs (Spetzler-Martin grades I and II), surgery has a high rate of cure with low complication rates and immediate elimination of hemorrhage risk. The experience and surgical performance of the operating team is essential for optimizing treatment outcomes. Studies have shown that the cure rate following surgery can be between 90 to 100%. These percentages are more attainable with lesions smaller than 3 cm. Furthermore, the risk of morbidity and mortality with low-grade lesions is less than 10%. As AVM grade increases, the likelihood of favorable outcome declines.
The rates of good outcomes vary according to several factors related to the patient and the AVM. Regarding seizure control, the best outcomes are achieved with complete AVM removal. Reports have shown that following complete surgical resection, around 80% of patients with a history of seizures are seizure-free following surgery. It should be emphasized that a multidisciplinary team approach that includes other specialists such as neurologists is recommended to optimize treatment outcomes and ensure the best patient care.
How Serious is AVM Surgery?
The risk of complications is decreased via thorough preoperative preparation, competent surgical technique and judgment, and excellent postoperative management. The decision to perform surgery should be individualized to each patient after a careful review of the indications for surgery. The use of new imaging technologies in combination with operative tools and surgical expertise can also promote good outcomes and decrease the risk of surgical complications.
Two common complications in AVM surgery are bleeding and brain tissue injury. Bleeding can occur directly from the lesion or the abnormal blood vessels around it. Brain tissue injury can occur mainly during AVM localization and resection. Optimal surgical planning and extensive surgical experience decrease these risks. The postoperative period is a delicate time where complications can arise. Therefore, the neurosurgical team will closely observe the patient to promptly identify and manage any clinical concerns.
Conclusions
Treating patients with brain AVMs requires a firm understanding of the disease and the pros and cons of each treatment modality. A multidisciplinary team approach favors the best treatment outcome. The best time for surgery depends on the patient's clinical condition and the characteristics of the AVM, with the primary goal of surgery being complete resection. Thorough preoperative planning, a competent surgeon with special expertise, and excellent postoperative care can minimize the risk of complications.
Key Takeaways
- Surgery involves opening the skull to reach the AVM with the goal of complete removal while avoiding damage to the surrounding brain tissue.
- The timing of surgery depends on the neurologic condition of the patient and the characteristics of the AVM.
- Complications such as bleeding and damage to the brain tissue are possible, but preoperative preparation and surgeon’s experience decrease the risk of their occurrence.











