Overview of Natural History of Glioma

Changes in the genetic material of cells (i.e., DNA) lead to the development of brain and spinal tumors like gliomas. Although the exact underlying cause of glioma development is unknown in most cases, common risk factors are exposure to ionizing radiation and hereditary genetic conditions.
Gliomas can be asymptomatic or symptomatic. Symptoms depend on location, size, and tumors’ aggressiveness. Diagnosis requires a detailed patient history and physical exam followed by imaging (MRI) testing. Obtaining a tumor sample via a biopsy procedure can be necessary to guide treatment. Surgical removal is usually the first line of treatment followed by radiation and chemotherapy.
Most risk factors for glioma development are not controllable. However, an early diagnosis, which is often not possible, can prevent the progression of a low-grade lesion into a highly aggressive high-grade tumor. Having a glioma does not mean you have cancer. Low-grade gliomas are generally noncancerous and carry a relatively good prognosis. Contrary to that, high-grade gliomas are cancerous; they grow fast and invade normal brain tissues faster and earlier. Gliomas are a broad category of brain tumors. Their natural history depends on specific patient and tumor characteristics.
Causes of Glioma
Following the diagnosis of a glioma, it is common for patients and caregivers to search for potential causes of gliomas. Unfortunately, the exact underlying cause of tumor development is unknown in most cases. It is believed that they arise due to the accumulation of genetic changes that cause the glial cells to lose their typical growth control pattern.
A normal glial cell will die and be replaced once it fails to work correctly. Contrary to that, when specific genetic alterations occur, cells become immortal and/or start to develop at a much faster pace. Hence, the tumor begins to grow. The most common potential risk factors are the exposure to ionizing radiation seen in atomic bomb survivors and hereditary genetic conditions.
Studies in rare genetic disorders such as Turcot syndrome, Neurofibromatosis type 1, and Li-Fraumeni syndrome have pointed out the association of genetic alterations to glioma formation.
It is relevant to point out that not all gliomas have the same behavior. For instance, less invasive tumors are low-grade, while more aggressive ones are high-grade. Sometimes, high-grade gliomas arise from low-grade lesions either as a transformation over time or as a recurrence after initial treatment. However, the sporadic appearance of high-grade lesions has also been observed. Remarkably, low-grade tumors have the best survival rates when diagnosed and treated.
Symptoms of Glioma
Gliomas can be asymptomatic or present with nonspecific symptoms that overlap with the presentation of other diseases. Symptoms of gliomas can be variable depending on the tumor's location, size, and aggressiveness. Symptoms arise due to the growth, infiltration, and compression of normal brain tissue around the tumor. The tumor can also increase the pressure within the skull, producing alterations in the brain's normal function.
The most common symptom presentations are recurring headaches, memory issues, personality changes, drowsiness, unprovoked vomiting, seizures, and in more advanced cases, decreased level of consciousness. Every brain and spinal cord region has a different function, so symptoms change depending on the area affected. High-grade gliomas produce symptoms that progress over days to weeks, whereas low-grade gliomas show symptoms over months to years.
Interestingly, the tumor location can determine the moment symptoms appear. Susceptible areas can produce symptoms earlier. The knowledge about the function of each brain area allows the physician to point specific symptoms to specific brain locations. Although symptoms can often be vague, learning about common symptoms can be a powerful tool for an earlier tumor diagnosis and recurrence identification.
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.

Diagnosing a Glioma
As I mentioned above, tumors of the brain and spinal cord can have symptoms that are not specific and overlap with other conditions. To diagnose a glioma, doctors will conduct a thorough workup in a stepwise approach that starts with extensive patient history, physical and neurological examination, followed by dedicated medical imaging and possibly tumor biopsy.
Even though the physical exam will not diagnose a glioma, it is fundamental to guide further diagnostic decisions. The next step is medical imaging with either a CT scan or an MRI. Contrast dye can be added to both imaging modalities. CT scans use X-rays; they are fast and painless, making them a common first step.
MRI studies use magnets and radio waves. Caution should be taken with implanted devices (i.e., pacemakers, defibrillators, etc.). They take longer (i.e., 30 to 45 minutes), which can be challenging for some patients to tolerate. Their advantage is the absence of X-rays and the clear and detailed images they produce. Depending on the case, the neurosurgeon can choose to extract a piece of the tumor (i.e., biopsy) for analysis via a short procedure. A biopsy can provide definitive information to focus the treatment approach. The diagnostic process can be challenging. Therefore, close communication between the healthcare team and the patient is fundamental.
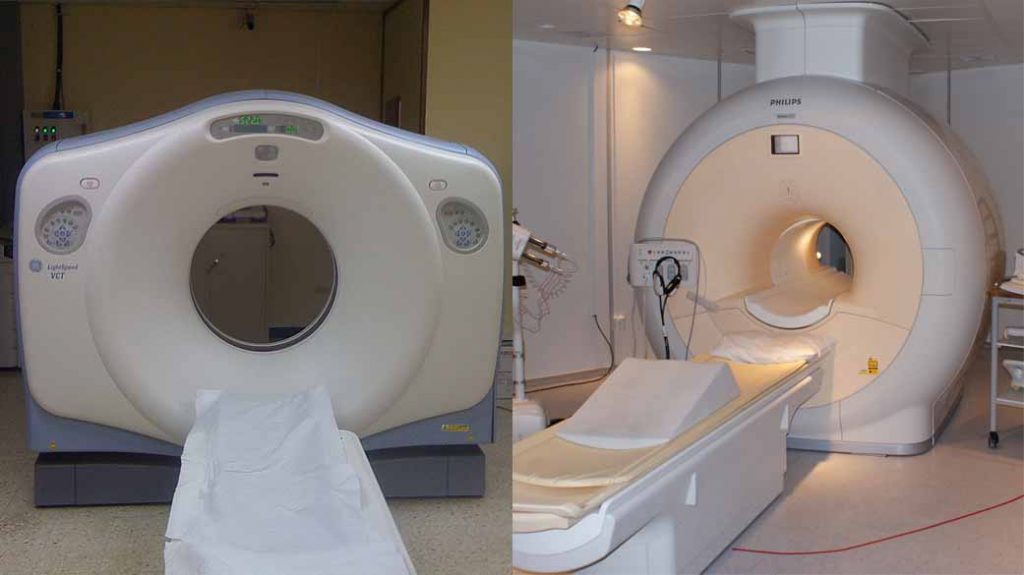
Figure 1: Examples of CT scan (left) and MRI (right) machines.
Preventing Glioma
No evidence has shown how to prevent a glioma from originating and developing. It is relevant to point out that risk factors do not cause diseases; they are common findings in people with specific conditions. Unfortunately, scientific studies are not conclusive to point out specific environmental risk factors to avoid. For instance, stress and anxiety have not been demonstrated to cause gliomas. As general advice, patients are suggested to practice a healthy lifestyle that includes adequate rest and sleep, balanced nutrition, and a regular exercise routine. Although to date, it is not possible to predict who will develop gliomas, the avoidance of risk factors is helpful but does not guarantee absolute protection.
Cancer and Glioma
Cancer and gliomas are not necessarily synonymous. Gliomas can be noncancerous (relatively benign) or cancerous (malignant). Symptoms and treatment selection are unique to the characteristics of the tumor and the patient. Malignant tumors are made up of cancerous cells.
Two fundamental features that malignant cells show are their high-speed growth pattern and their capacity to invade normal tissues. Glioma grading determines the severity of the lesion based on microscopic observation of the tumor cells. Low-grade tumors are generally considered noncancerous, and their cells have minimal alterations and low invasion capability. Typically, they have a good prognosis.
On the other hand, high-grade tumors are fast-growing and invasive. Two common examples are glioblastoma and anaplastic astrocytoma. Moreover, the prognosis tends to be poor for high-grade tumors. Although gliomas can behave differently according to their grade, communication between the healthcare team and the patient is critical.
To summarize, the exact underlying cause of glioma development is not known. Risk factors that increase the probability of accumulating genetic mutations are the most commonly associated with tumor development. Even though symptoms are nonspecific, early healthcare evaluation and management is a priority to avoid tumor progression and transformation into a highly aggressive variant.
Initial imaging studies followed by tumor biopsy are essential steps to guide therapy. Not all gliomas are cancerous. Lower-grade tumors have the best prognosis if diagnosed and treated early. Professional healthcare communication and advice is always the best option to achieve the best treatment outcomes.
Key Takeaways
- The accumulation of genetic mutations can lead to the development of brain and spinal cord gliomas. Potential risk factors for glioma development are exposure to ionizing radiation and hereditary genetic conditions.
- Gliomas can be asymptomatic or symptomatic. Common symptom presentations are recurring headaches, personality changes, and seizures.
- Diagnosis is made with detailed patient history and physical exam, followed by imaging studies. Finally, a biopsy of the mass will specifically direct treatment.
- There is no evidence to show how to prevent gliomas.
- Not all gliomas are cancer. Low-grade lesions carry the best prognosis.











