Overview of Acoustic Neuroma Survival

An acoustic neuroma, or vestibular schwannoma, is a benign tumor that grows on the eighth cranial nerve (also known as vestibulocochlear nerve). As it grows, it can press against structures in and around your vestibulocochlear nerve, causing hearing loss, tinnitus, and balance problems.
If one becomes large enough, it can also cause a buildup of cerebrospinal fluid (CSF) within the brain leading to increased pressure (hydrocephalus) and can even put pressure on the brainstem. With those symptoms, it's understandable that receiving an acoustic neuroma diagnosis would cause concern.
Fortunately, the prognosis for this condition is generally favorable. Acoustic neuromas grow slowly and many are asymptomatic. Still, the primary worries for most patients are about the long-term outlook and quality of life. This article will provide basic information on what to expect for patients living with acoustic neuromas as well as the recovery outlook for those after treatment.
Surviving an Acoustic Neuroma
Upon diagnosis with an acoustic neuroma, you may wonder whether you can survive the condition without life-altering effects. Acoustic neuromas are not cancerous, so there is no risk of them spreading to other body parts. They can, however, cause problems as they grow larger.

Figure 1: MRI of a patient’s brain with a large acoustic neuroma (left) and a drawing of a large acoustic neuroma pressing on surrounding brain structures (right).
With proper treatment and monitoring, a poor prognosis from an acoustic neuroma is extremely unlikely. Hearing loss is one of the most common symptoms of an acoustic neuroma and can impact the quality of life for patients. In extremely rare cases, large acoustic neuromas can push against your brainstem (the critical part of the brain where your spinal cord connects to your brain) which can cause neurological deficits and even block the flow of cerebrospinal fluid (CSF). This blockage can lead to hydrocephalus, a buildup of fluid in the cavities of the brain that can lead to the following symptoms:
- Headache
- Blurred or double vision
- Nausea or vomiting
- Poor coordination and balance
- Changes in mood
- Difficulty sleeping or remaining awake
- Loss of mobility
- Speech difficulties
- A decline in memory, concentration, and other cognitive skills
Hydrocephalus presents the most serious risk for patients with acoustic neuromas but it is very rare. Fortunately, acoustic neuromas grow at a slow rate. In addition, most neuromas don't develop large enough to threaten the brainstem.
Why should you have your surgery with Dr. Cohen?
Dr. Cohen
- 7,500+ specialized surgeries performed by your chosen surgeon
- More personalized care
- Extensive experience = higher success rate and quicker recovery times
Major Health Centers
- No control over choosing the surgeon caring for you
- One-size-fits-all care
- Less specialization
For more reasons, please click here.
How Effective Is Treatment?
Several treatment strategies exist for acoustic neuromas and depend largely on the size of the tumor, the age and health of the patient, and types of symptoms the patient is experiencing.
Surgery by way of craniotomy is the most common treatment for a growing or large acoustic neuroma. There are several surgical approaches your surgeon may consider, including the retrosigmoid, middle fossa, and translabaranthine approaches.
Each approach has advantages and disadvantages that must be carefully considered to maximize outcomes. Surgery does carry the risk of worsening symptoms of facial nerve weakness. Sometimes it is unsafe to remove the entire acoustic neuroma as the tumor is very adherent to the facial nerve. Leaving behind even a small section of the tumor can increase the chance of recurrence down the line. Despite this, only 30% of patients experience recurrence after four years following surgery. Radiation is an excellent option to prevent the small tumors or residual tumors after surgery from growing.
Radiation therapy is also a possible treatment option. Often used as primary treatment for small tumors or as post-operative adjuvant, radiation therapy prevents recurrence by destroying most of the remaining tumor cells. In well selected patients, radiation therapy has an extremely small chance of damaging healthy brain tissue or risk of future tumors around the area being treated.
If the acoustic neuroma is small and asymptomatic, your surgeon may recommend for observation, taking a "watch and wait" approach to determine whether the tumor will require treatment in the future. You may be required to undergo regular surveillance imaging to monitor for any changes every 12 months using an MRI. Some patients elect for observation if the growth is small and does not adversely affect a patient's hearing, balance, or other functions.
Follow-up Care for an Acoustic Neuroma
Living with an acoustic neuroma can have an impact on a patient’s quality of life, however this can be minimized with early diagnosis and appropriate treatment. Follow-up care is vital to monitor for changes, especially after treatment. Even after a tumor is removed, there is a chance, albeit small, of recurrence. Lingering side effects may also occur after treatment. Serial MRIs are needed at regular intervals for the patients wishing to monitor a small and asymptomatic tumor.
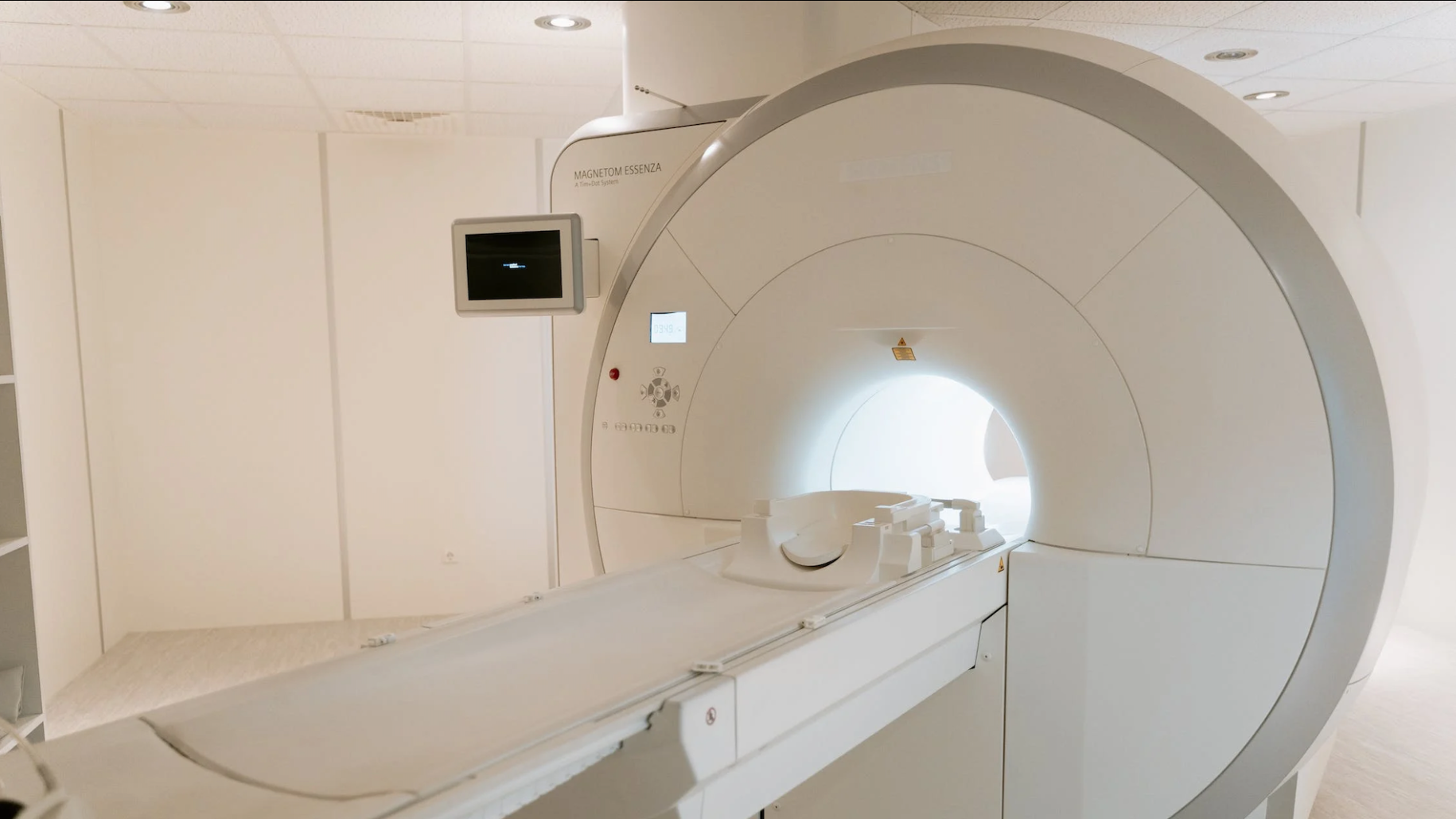
Figure 2: Magnetic resonance imaging (MRI) are the best diagnostic imaging for acoustic neuromas and are often used to monitor for growth in asymptomatic patients with small tumors.
Treatments for acoustic tumors are likely to cause significant decline in your hearing. Large tumors often have caused hearing loss by the time of the tumor diagnosis. There are several options available to mitigate the challenges caused by hearing loss on one side. Please note that one-sided hearing loss will not allow you to recognize the direction of the sound and therefore you will not be able to understand the position of the source of any sound:
- Cochlear implants can help restore a patient's hearing. Sometimes, a surgeon can insert the implant during the same surgery used to remove the acoustic neuroma, ensuring only a brief adjustment period following treatment.
- If the surgery for the tumor has been a while ago and therefore there is already facial muscle impairment, facial reanimation surgery is an option for achieving a reasonable cosmetic result.
- Physical therapy can help restore/improve the patient's balance.
Key Takeaways
An acoustic neuroma is a rare condition, occurring in one in 100,000 people yearly. In many cases, the tumor doesn't grow large enough to cause symptoms, meaning that individuals can go for years without knowing that they have an acoustic neuroma.
With proper diagnosis and treatment, the prognosis for an acoustic neuroma is overwhelmingly positive. However, even with treatment, it's necessary to continue to manage symptoms and postoperative effects. Living with an acoustic neuroma is possible with very few changes to your quality of life. Many patients have experienced acoustic neuroma treatments and continue working, exercising, and living normal lives for years thereafter.
Key Takeaways
- Acoustic neuromas grow at a slow rate, so they often don't manifest symptoms until they reach a reasonable size.
- The general prognosis for the condition is typically favorable, as acoustic neuromas are rarely ever life-threatening.
- The most significant risk associated with acoustic neuromas is their growth placing pressure on vital structures such as the brainstem.
- Ongoing management of symptoms and effects from treatment is necessary to maintain a good quality of life.
- After treatment for an acoustic neuroma, there are options for restoring the patient's hearing and balance.











